Since the launch of the COVID Confirmed (COCO) Clinic in early April, over 4,700 patients with COVID-19 have been given virtual follow-up services after being discharged from the hospital. Not only has this virtual outpatient clinic helped patients on their road to full recovery and often kept them from being readmitted to the hospital, it also provided resident physicians and senior medical, nurse practitioner, physician assistant, PharmD, social work and behavioral health students, with a place to complete their clinical rotations. In mid-March, the Association of American Medical Colleges (AAMC) issued new guidance for medical student clinical rotations during the coronavirus which stated that it, “strongly supports medical schools pausing all student clinical rotations, effective immediately, until at least March 31,” due to concerns about the availability of personal protective equipment (PPE) and to give time for appropriate educational strategies and alternative clinical experiences to be developed and implemented.
Volunteers and trainees played vital roles within the clinic which included conducting regular welfare checks, offering support and discussing any symptoms that haven’t been resolved. Social work and behavioral health students were not originally part of the COCO Clinic when it first launched, but the team quickly realized that COVID-19 and quarantine could severely impact a patient’s mental health and so the interprofessional team expanded. The medical, social, and mental health assessments screened for depression, anxiety and substance abuse, and if a patient answered “yes” to any of the questions, they were offered resources or referrals to support. According to Asa Oxner, MD, FACP, COCO Clinic operations director, one patient agreed to being referred to the mental health team of COCO and a real suicide attempt was mitigated.
In addition to regular follow-up assessments, nurse practitioner students were in charge of monitoring the dashboard that displays the oxygen levels and heart rates of high-risk patients who were wearing a special device on their wrist.
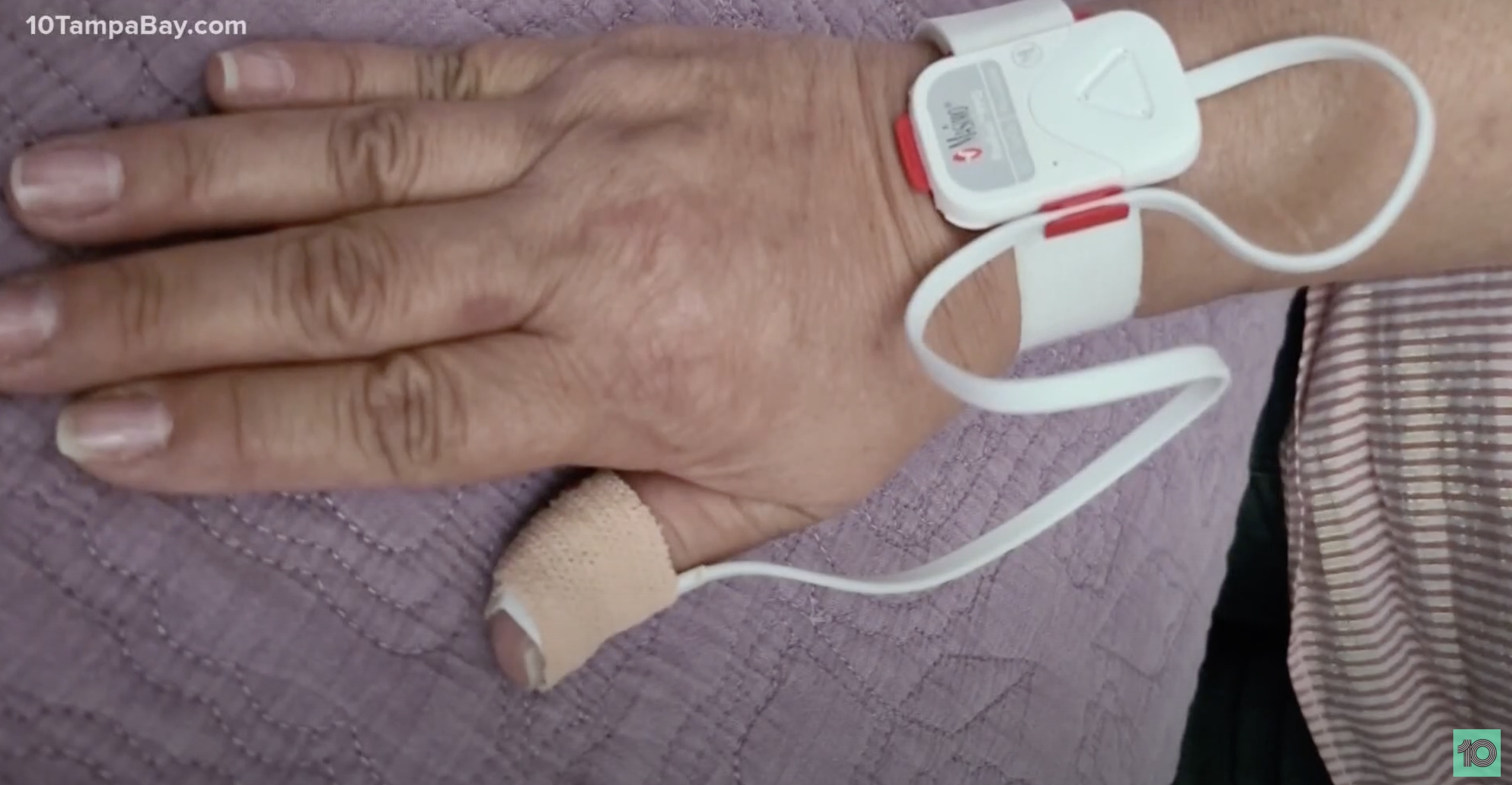
A patient wearing one of the COCO Clinic’s monitors. Photo by CBS affiliate, 10 Tampa Bay, from their, “COVID-19 Telehealth Clinic Getting Overloaded with Tampa Bay Patients” video.
“Volunteering with the clinic has been a unique educational experience. The clinic administrators do a great job of turning every opportunity into a teaching moment,” said Joshua Mizels, Morsani College of Medicine fourth-year medical student and past clinic volunteer. “My classmates who all volunteer have had the opportunity to keep interacting with patients, giving us the opportunity to learn more about what they are going through during this pandemic. The experience from this opportunity has been invaluable toward my medical education. ”
Lucy Guerra, MD, MPH, FACP, and Asa Oxner, MD, FACP, co-coordinators of the COCO Clinic, along with Elimarys Perez-Colon, MD, medical director, Christine Jennings, RN, nurse manager, and Rachelle Idziak, MD, data manager, led the effort to get the clinic up and running and play a pivotal role in helping the community. For their dedicated efforts, the doctors received a USF Health Culture Coin from Chief Medical Officer, Dr. Mark Mosely.

Dr. Asa Oxner (left) and Lucy Guerra (right), COCO Clinic co-coordinators, were presented with USF Health culture coins by Dr. Mark Moseley, USF Health chief medical officer, for leading efforts to get the virtual clinic up and running.
“We have been successful in offering close follow up to patients keeping them out of the hospital when able, monitor patient’s vital signs remotely to identify patients at higher risk, safely linking patients to care and offering education and reassurance to patients with COVID19 in the Hillsborough county,” said Dr. Elimarys Perez-Colon, assistant professor of medicine, vice chief of medicine at Tampa General Hospital, and medical director of the COVID-19 Confirmed Clinic. “The data collected will assist our department of health to better understand the distribution and epidemiology of COVID19 in our county. This effort wouldn’t have been successful without the assistance and compassionate care offered by our trainees.” In the first three months, over 150 trainees played a part in the care of patients.
The COCO Clinic has been the talk of the town, featured in news stories by ABC Action News, Baynews 9, 10 Tampa Bay, among others.
After the success of the virtual clinic for COVID-19 patients, clinic leaders began working with partners at Tampa General Hospital and the Florida Department of Health to make the clinic a permanent resource for the community. As of November 12th, the COCO Clinic transitioned management of the clinic to TGH and became the TGH Transitional Care Center. “This transition will allow the clinic to continue operating and provide excellent care to our patients impacted by COVID-19, while allowing USF Quality and Clinical Operations Department staff who have been assisting the COCO clinic to return to their normal non-COVID duties,” said Dr. Moseley. “The clinic will continue to provide hours to our medical, pharmacy, and nurse practitioner students and our teaching attendings will continue to support the clinic. TGH has also been able to hire several RNs and Mas, who have been training in the current clinic and will be able to facilitate a smooth transition.” An emphasis will be put on taking care of COVID-19 ‘long haulers,’ virus survivors who continue to have side effects weeks, or months, after surviving the coronavirus. Caring for these patients will also help conduct research into the little known long term effects of COVID-19. Beyond COVID-19, the clinic can continue to help patients using the same monitoring and staffing model, but for serious chronic diseases such as heart failure or chronic obstructive pulmonary disease (COPD).
